- Details
- Hits: 1904
Table of Contents
Commercials created by The Doctor Patient Forum
Statements/Corrections that have been made (we have contributed to making this happen)
Podcasts or shows DPF has been featured on
Articles that have mentioned The Doctor Patient Forum/Don't Punish Pain Rally or quoted us
Articles we helped research or write
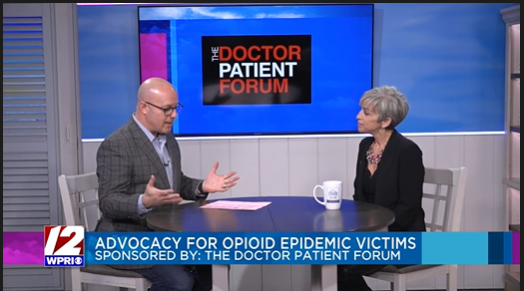
Studio 10 segment with Claudia Merandi
The Rhode Show with Claudia Merandi - 1/24/24
- Details
- Hits: 2407
Claudia has Crohn's Disease. She was able to be part of a fitness competition on 11/19/22 and used her platform to bring awareness to the untreated pain crisis in America. She brings awareness to patient abandonment and suicide due to untreated pain.
- Details
- Hits: 1960
Commercial for Providers
Commercial for Pain Patients
- Details
- Hits: 2182
- The Pain Was Unbearable, So Why Did Doctors Turn Her Away? - NarxCare
- US Could Loosen Some Restrictions on Prescribing Opioids - CDC Guidelines, CPP discrimination
- Medical Racism is Fueling the Black Overdose Crisis, Advocates Say -12/20/21
- I've Been a Nurse for 30 Years. Opioids Saved my Patients' Lives - Beth Dost/DPF Board Member - 5/6/23
- FDA weighs when software becomes a medical device - NarxCare - 5/26/23
- When does software cross the line and become a medical device? - NarxCare - 6/8/23
- Artificial Intelligence May Influence Whether You Can Get Pain Medication - NarxCare -8/23/23
- Ohio pain patients join nationwide effort to scale back restrictions on opioid prescriptions - 10/3/23
- Hidden Formulas, High Stakes: The Fight to Regulate Clinical Decision Support Tools pdf - 5/22/25
- Details
- Hits: 1418
- Roger Chou’s Undisclosed Conflicts of Interest: How the CDC’s 2016 Guideline for Prescribing Opioids for Chronic Pain Lost Its Clinical and Professional Integrity
- Undisclosed Conflicts of Interest by Physicians Creating the CDC Opioid Prescribing Guidelines - Bad Faith or Incompetence?
- Undisclosed Conflicts of Interest by Physicians Creating the CDC Opioid Prescribing Guidelines - An Epilogue
- The Doctor Patient Forum's Comment on the Docket of 2022 CDC Guideline Draft